Insurance
Cyber Insurance Coverage with Silverfort: Protecting Your Digital Assets

Cyber Insurance Coverage with Silverfort, the rate at which cyberthreats are developing is startling, making them a major concern for companies of all kinds. Protecting vital information and daily operations has never been more important for businesses in the age of the internet. Cyber insurance is a preventative measure that can lessen the impact of monetary losses and legal obligations after a cyber attack. Silverfort is a state-of-the-art cybersecurity system that we’ll examine in detail as we explore the realm of cyber insurance coverage.
Introduction to Cyber Insurance
(Cyber Insurance Coverage with Silverfort)
With so many cyber dangers out there, it may be difficult for organisations to protect their data. In the case of a data breach or other cyber disaster, cyber insurance can serve as a financial safety net. It’s an important part of any plan to reduce the impact of cyberattacks on an organisation.
Understanding Silverfort
Silverfort is a market-leading cybersecurity solution that gives businesses a leg up in terms of protecting their data. Access to sensitive systems and data is restricted to authorised users thanks to its adaptive authentication and threat detection features. Its risk-based procedures and multi-factor authentication are crucial in keeping out intruders.
The Need for Cyber Insurance Coverage
Cyber insurance is becoming increasingly important as both the frequency and complexity of cyberattacks rise. No system, no matter how well protected it is, can ever be 100% safe. Faster recoveries from cyber attacks are covered by insurance, which helps businesses save money and salvage their reputations.
Silverfort’s Key Features
Silverfort’s major attributes make it more appealing to enterprises.
- Adaptive Authentication,
- Threat Detection,
- Risk-Based Policies,
- Identity Verification are some of these characteristics.
Choosing the Right Cyber Insurance Policy
It is critical to match the coverage of your cyber insurance policy with your organization’s unique requirements and exposures. Data breach notification fees, legal fees, and lost business income should all be covered by your insurance coverage. You may modify the coverage to fit your needs with the advice of insurance experts.
Benefits of Silverfort for Businesses
Silverfort’s offerings go above and beyond conventional cyber defences. It aids firms in strengthening their defences, making it more likely that they will be able to rapidly recover from any attacks. This, in turn, reduces the cost and disruption of a cyber attack.
The Growing Threat of Cyberattacks
Businesses nowadays must change along with the ever-evolving nature of cyber threats. Cyberattacks are becoming increasingly common, and their effects may be catastrophic. Silverfort is an essential component in improving a company’s security.
Silverfort’s Unique Security Solutions
Silverfort’s one-of-a-kind method of providing safety sets it apart. It identifies and prevents unauthorised entry by integrating adaptive authentication with real-time threat detection. Its risk-based controls restrict access to private data to known, authorised individuals only.
Cyber Insurance and Regulatory Compliance
Data protection and cybersecurity must meet high regulatory criteria in many sectors. The danger of fines and legal trouble can be minimised with Silverfort’s assistance in maintaining compliance with these requirements.
How Silverfort Mitigates Risks
By limiting access to confidential information to those with proper authorization, Silverfort adds another layer of protection. It prevents security holes from being exploited by keeping a close eye on user actions and instantly reacting to those that seem suspect.
Evaluating Cyber Insurance Costs
Cyber insurance premiums differ in price based on factors such as policy limits, company size, and business sector. When choosing an insurance, it’s important to consider both the premiums and the expenditures that might result from a cyber attack.
The Role of Silverfort in Incident Response
Should a cyber incident occur, Silverfort’s skills will be crucial in dealing with the aftermath. Damage and restoration time can be reduced if hazards are quickly identified and contained.
The Future of Cyber Insurance
Cybersecurity is a constantly changing field. Businesses will need cyber insurance even more in the future. The constant development of Silverfort ensures that it will always be one step ahead of new dangers.
Conclusion (Cyber Insurance Coverage with Silverfort)
In conclusion, Silverfort-specific cyber insurance is a critical component of today’s company risk management. You cannot overstate the need to adequately protect your company’s digital assets in the face of increasingly sophisticated cyber attacks.
FAQs (Cyber Insurance Coverage with Silverfort)
- What is cyber insurance coverage?
- Cyber insurance coverage is a policy that provides financial protection to businesses in the event of a cyber incident or data breach.
- How does Silverfort enhance cybersecurity?
- Silverfort enhances cybersecurity by providing adaptive authentication, threat detection, and risk-based policies to prevent unauthorized access.
- What should businesses consider when choosing a cyber insurance policy?
- Businesses should consider their specific vulnerabilities, regulatory requirements, and the potential financial impact of a cyber incident when choosing a policy.
- How does Silverfort help with regulatory compliance?
- Silverfort helps businesses stay compliant with data protection regulations by ensuring that only authorized users access sensitive data.
- Why is the future of cyber insurance important for businesses?
- The future of cyber insurance is important because cyber threats are continuously evolving, and having the right coverage is crucial for business continuity and protection.

Insurance
How proper training in cardiology and dermatology billing services can minimize claim denials and delays
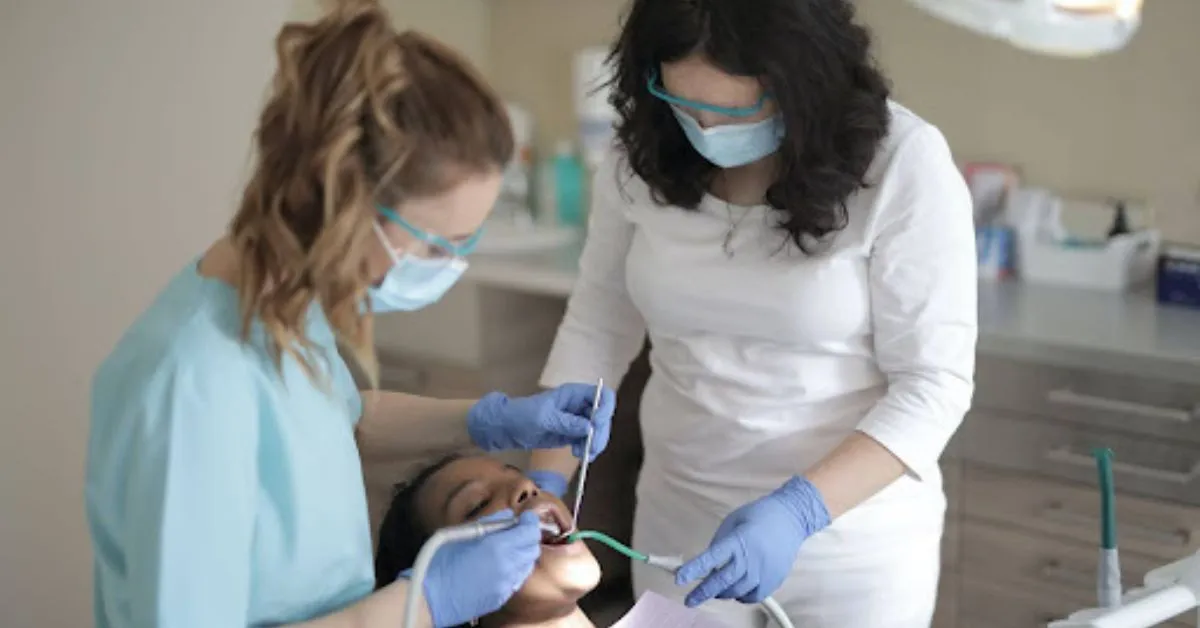
The medical billing process is intricate, involving a comprehensive understanding of coding systems, insurance policies, and healthcare regulations. In specialties like cardiology and dermatology, the complexity of procedures and varying insurance requirements increase the likelihood of claim denials and delays. Proper training for billing personnel is crucial to reduce errors and streamline the claims process. This article explores how effective training in cardiology billing services and dermatology billing services can minimize claim denials and delays.
Understanding the Causes of Claim Denials and Delays
Claim denials and delays can occur for various reasons, often rooted in administrative errors, incorrect coding, or failure to comply with insurance guidelines. Understanding these causes is the first step in addressing them.
Common Reasons for Claim Denials
- Incorrect or Missing Information: Inaccuracies in patient information, insurance details, or procedural codes can lead to claim rejections.
- Invalid or Outdated Codes: Using outdated medical codes or codes that do not align with the procedure can result in denial.
- Lack of Medical Necessity: If the insurance company deems a procedure unnecessary, the claim can be denied.
Factors Contributing to Claim Delays
- Complex Claim Processing: Cardiology and dermatology procedures often require more detailed information, which can slow down claim processing.
- Administrative Backlogs: High volumes of claims with manual processing can lead to delays.
- Incomplete Documentation: Missing supporting documents can cause insurers to request additional information, delaying the claim approval process.
The Role of Training in Reducing Errors
Proper training is essential for billing personnel to understand the intricacies of cardiology and dermatology billing services. Well-trained staff can identify and correct potential issues before submitting claims, reducing the likelihood of denials and delays.
Comprehensive Knowledge of Medical Codes
Cardiology and dermatology billing require familiarity with specific coding systems like CPT (Current Procedural Terminology), ICD (International Classification of Diseases), and HCPCS (Healthcare Common Procedure Coding System). Proper training ensures that billing staff understand the correct codes to use for different procedures and diagnoses.
Staying Updated with Regulations and Insurance Policies
Insurance policies and healthcare regulations are constantly evolving. Billing staff must stay informed about these changes to avoid errors in claim submissions. Proper training includes regular updates on new regulations and insurance requirements, ensuring compliance and reducing claim denials.
Improving Communication and Collaboration
Training in billing services also focuses on enhancing communication among different departments and with insurance companies. Better communication can help resolve issues that might lead to claim denials or delays.
Collaborating with Healthcare Providers
Billing staff need to work closely with healthcare providers to ensure accurate coding and proper documentation. Proper training includes communication skills that facilitate effective collaboration, allowing billing personnel to clarify doubts and gather necessary information.
Streamlining Communication with Insurance Companies
Establishing clear communication channels with insurance companies is crucial for resolving claim-related issues. Proper training helps billing personnel understand the best practices for communicating with insurers, reducing delays due to miscommunication or unclear documentation.
The Impact of Training on Patient Experience
Proper training in cardiology and dermatology billing services not only minimizes claim denials and delays but also improves the overall patient experience. Patients expect their claims to be processed efficiently, and any delays or denials can lead to frustration and dissatisfaction.
Ensuring Accurate and Timely Billing
When billing personnel are well-trained, they can ensure accurate and timely claim submissions. This reduces the risk of billing errors that could lead to financial stress for patients and contributes to a smoother healthcare experience.
Reducing Administrative Burdens for Patients
Claim denials and delays often require patients to navigate complex administrative processes to resolve issues. Proper training reduces these occurrences, easing the administrative burden on patients and allowing them to focus on their health and recovery.
Reducing Financial Losses and Improving Revenue Cycle Management
Effective training in cardiology and dermatology billing services plays a crucial role in reducing financial losses due to claim denials and delays. Incorrect or rejected claims can lead to lost revenue and increased operational costs. Proper training can help improve revenue cycle management by ensuring that claims are processed accurately and quickly, leading to better financial stability for healthcare providers.
Ensuring Consistent Cash Flow
Accurate and timely billing is critical for maintaining a consistent cash flow in medical practices. Proper training ensures that billing personnel can quickly resolve any issues related to claim denials, leading to faster reimbursements. This consistency in cash flow contributes to the financial health of cardiology and dermatology practices, allowing them to focus on patient care and service quality.
Reducing Costs Associated with Rework and Appeals
Claim denials often require rework, additional documentation, or formal appeals, which can be costly and time-consuming. Proper training reduces these costs by minimizing the need for rework and ensuring that claims are submitted correctly the first time. This not only saves time but also reduces administrative overhead, leading to greater efficiency in the revenue cycle.
Boosting Employee Morale and Productivity
The impact of proper training extends beyond reducing claim denials and delays; it also affects the morale and productivity of billing personnel. A well-trained team is more confident and efficient, leading to a positive work environment and better results.
Empowering Billing Staff with Knowledge and Skills
When billing staff are thoroughly trained, they are more likely to feel empowered and capable of handling the complexities of cardiology and dermatology billing services. This empowerment fosters a sense of ownership and pride in their work, leading to higher productivity and better outcomes for the organization.
Reducing Stress and Burnout
Claim denials and delays can create a stressful work environment, contributing to burnout among billing personnel. Proper training helps reduce stress by equipping staff with the tools and knowledge they need to navigate challenges effectively. This, in turn, leads to lower staff turnover, higher job satisfaction, and a more harmonious workplace.
Conclusion: The Importance of Ongoing Training
Proper training in cardiology and dermatology billing services is essential for minimizing claim denials and delays. It provides billing personnel with the knowledge and skills to navigate the complexities of medical coding, insurance
Insurance
The Importance of Dental Coverage

Providing all-inclusive benefits can be difficult for small business owners, mainly when staying profitable is essential. But offering dental insurance goes beyond being a nice-to-have; it’s vital to your workers’ general health and well-being. Dental insurance is a preventive measure that can save employers money and employees’ health because dental problems can cause or worsen other health problems.
A dental insurance plan can also be a robust recruitment and retention tool, helping small businesses stand out in a competitive labor market. Employees often view dental coverage as a demonstration of their employer’s investment in their health and quality of life. Thus, by offering dental benefits, small businesses can create a supportive work environment and foster loyalty and satisfaction among their workforce.
Understanding Dental Insurance Plans
PPOs, HMOs, indemnity plans, and discount plans are just a few different dental insurance plans. Each type can be chosen according to the particular requirements of your company and employees and offers a distinct approach to premiums, deductibles, co-pays, and provider networks.
It is essential to comprehend the subtleties of these plans. For example, PPOs generally offer a broad network of dentists and a balance between out-of-pocket costs and monthly premiums. In contrast, HMOs might offer lower premiums but with more limitations on provider choices. Indemnity plans provide a high degree of freedom in choosing dentists but often come with higher costs. Discount plans are not insurance per se but provide discounts on dental services from specific providers.
Choosing the Right Dental Plan for Your Business
Assessing your employees’ needs and preferences is the first step in selecting a dental plan. Consider factors such as the age demographics of your workforce, their general dental health, and the potential demand for specialized dental services. Additionally, evaluate the financial health of your business and determine how much you can contribute to the premiums. Conducting an employee survey to gather input on their dental insurance priorities may be valuable.
Comparing plan structures and benefits allows you to align your choice with those needs and preferences. Depending on the diversity of needs in your workforce, you may offer a single plan or a selection of plans. As you scrutinize potential plans, carefully reading the fine print can prevent surprises regarding coverage limits and exclusions.
Dental insurance for small business offers a valuable benefit to employees, promoting oral health and providing financial assistance for routine checkups, treatments, and emergencies.
Employee Engagement and Education
Employees need to comprehend their dental benefits to use them effectively. Develop educational materials that explain how dental insurance works, the process for claiming benefits, and the importance of preventative care. Consider hosting informational sessions and providing resources that answer common questions. Emphasizing the value of dental insurance in these communications can boost appreciation and engagement.
Facilitate a two-way dialogue where employees can ask questions and provide feedback on their experiences with the dental plan. This can highlight areas for improvement and ensure that the benefits meet their needs.
Cost Management and Budgeting
Financial planning for dental benefits is essential to avoid strain on your business’s resources. Establish a budget for dental insurance that factors in not only the premiums but also the potential costs of out-of-pocket expenses and co-pays for employees. This helps prevent unexpected financial burdens and ensures the sustainability of the plan.
Negotiating with insurance providers or exploring group rates can lead to more favorable terms. It’s also wise to revisit the dental insurance costs during each renewal period to identify any cost-saving opportunities that may have emerged.
Working with Providers
Selecting a dental insurance provider is as important as choosing the plan—research providers with a positive track record of customer service and claims processing. Establishing a direct line of communication with your provider can ensure swift resolution of any issues and facilitate handling employee claims.
Building a relationship with your provider can also provide you with industry insights and access to additional resources that can be shared with your employees to improve their usage of dental benefits.
Integration with Wellness Programs
Dental health should be considered part of a broader wellness strategy. Integrating dental coverage with other health and wellness initiatives can reinforce the importance of oral health as part of overall health. Offering incentives for regular dental checkups or including dental health challenges in your wellness programs can encourage better utilization of dental benefits.
This holistic approach shows employees that their total well-being is valued and can result in a healthier workforce.
Encouraging Benefits Utilization
Underutilized benefits are benefits-spent. Ensure that employees know the full scope of their dental coverage, including routine checkups and cleanings, often covered at little to no cost. Motivate employees to take preventive measures by emphasizing regular dental care’s long-term health and financial benefits.
Keep track of the utilization rates and share these figures with staff. If rates are low, investigate why and adapt your strategy to improve the numbers. Better utilization can lead to a healthier workforce and potential savings for your business through reduced healthcare costs.
Reviewing and Adjusting the Plan
Periodically reviewing your dental plan can ensure it remains competitive and meets your employees’ needs. Market trends and healthcare costs change, as do the dental needs of your workforce.
Be open to adjusting the plan structure, coverage levels, or provider networks as these factors evolve. Employee feedback gathered during the year can inform these modifications, ensuring that changes are meaningful and responsive to their preferences.
Leveraging Technology in Dental Benefits Administration
Technology can significantly streamline the administration of dental benefits. These tools can simplify processes and increase efficiency, from enrollment systems to mobile apps that help employees track their benefits.
Investing in a robust benefits administration platform can save time and reduce errors, leading to a better experience for employees and your HR team. These systems can also provide analytics to help track utilization and cost trends, guiding future benefit decisions.
Further Resources and Expert Insights
Regularly consult resources such as industry publications, webinars, and professional networks to maintain a solid understanding of dental benefits. Expert insights can spotlight emerging trends and advise on managing the complexities of offering dental insurance in a small business setting. Attending conferences or engaging with industry experts can expand your knowledge and provide new perspectives on effectively delivering your employees the best dental insurance coverage.
Insurance
Mental Health Care: Can Everyone Afford to Get Help?

Key Takeaways
- Understanding mental health insurance coverage is essential for accessing quality care.
- Navigating insurance can be complex, but there are resources and strategies to help.
- Mental health parity laws aim to ensure fair coverage for mental health treatment.
- The interplay between insurance policies and mental health services is constantly evolving, notably with the rise of telehealth.
Understanding Mental Health Coverage
Regarding mental health, the role insurance plays cannot be understated. Each policy provides a roadmap of benefits, but the complexity often lies in the specifics—what treatments are covered, the extent to which therapy is included, and whether there’s a cap on the number of covered sessions. To navigate such a landscape effectively, one must become fluent in the language of insurance plans and patient benefits. Often, this involves familiarizing oneself with industry terminology, such as co-pays, co-insurance, and the nuances of coverage limits.
In therapy, understanding the critical distinction between in-network and out-of-network providers is integral to managing healthcare costs. Opting for an in-network therapist often translates to lower out-of-pocket costs, thanks to predetermined rates established with insurers. However, selecting an out-of-network physician could increase costs because these therapists have yet to reach a rate agreement with insurance companies, so consumers must deal with potential reimbursement procedures.
Navigating Insurance for Therapy
Delving into mental health care starts with thoroughly assessing one’s insurance benefits. Ensuring that essential treatment like therapy is covered requires a proactive approach—contacting one’s insurer, inquiring about the specifics of coverage, and understanding the extent of the services accessible under one’s plan are all essential steps. For Seattle residents, finding comprehensive service providers such as Aetna therapy in Seattle might prompt a closer look at how in-network therapists can reduce out-of-pocket costs.
Insurance can be bewildering, with its myriad of terms and varying levels of coverage. Educating oneself on personal insurance specifics is critical. Only some people have the luxury of choosing various therapeutic approaches, but knowing one’s insurance plan can open up possibilities and lead to the right fit for one’s psychological well-being.
Health Insurance’s Impact on Mental Health Services
One’s health insurance can significantly influence access to mental health services and the ability to maintain continuous care. According to statistical statistics, those with insurance are more likely to seek out and make use of mental health services. Moreover, insurance facilitates ongoing care, often necessary for effective mental health treatment. The process of utilizing insurance for therapy can sometimes be grueling, and navigating approval and claims may seem like a puzzle to many individuals seeking treatment.
Varying degrees of coverage, claim processes, and the overall user-friendliness of insurance programs strongly shape patient experiences. An insured individual’s journey may include choosing the right therapist—one who aligns with their therapeutic needs and their insurance plan. Solely for illustration, while exploring services like Seattle Aetna therapy, the importance of checking whether potential therapists accept your insurance plan becomes clear.
Challenges Faced by Patients and Providers
Patients looking for mental health services via their insurance might encounter several obstacles along the way. Claim denials, discrepancies in billing, or disputes about what constitutes ”medically necessary” treatment can hinder the journey to obtaining treatment. Mental health providers, too, face significant challenges; the administrative burden of dealing with insurance requirements, such as obtaining prior authorizations and submitting claims, can detract from clinical care. The balance between ensuring administrative compliance and focusing on the therapeutic process can be delicate on both fronts.
Strategies for Managing Costs With and Without Insurance
Financial planning for therapy can be approached from several angles. Understanding coverage nuances, such as meeting deductibles and out-of-pocket maximums, is crucial for those with insurance. However, affordability becomes an even more pressing concern for individuals with little to no insurance. Thankfully, there are options out there. Many therapists provide sliding scale pricing depending on a person’s financial situation. Nonprofit groups may give treatments for free or at a significantly discounted rate. Community health centers also often have programs or partnerships to make therapy more accessible to the financially vulnerable.
Mental Health Parity Laws
Advocacy for equal coverage of mental health services has led to establishing mental health parity laws. Such legislation prevents health insurance plans from imposing more restrictive conditions on mental health benefits than on medical or surgical benefits. These regulations have significant ramifications since they aim to end prejudice and mainstream mental health services as essential components of general health. These legal developments have culminated in the attempts to recognize and solve the need for equitable mental healthcare in our healthcare systems.
Future of Insurance Coverage for Mental Health
The ever-evolving relationship between health insurance policies and mental health services has seen significant transformations in recent years, particularly with the emergence of telehealth. This advancement has spearheaded a new era in healthcare, offering remote access to therapy and other mental health services. Insurance providers are adapting to these changes, re-evaluating coverage policies to more inclusively accommodate teletherapy and other digital health services. The ripple effects of these evolutions signify a broader, more accessible scope of mental health care coverage moving forward.
As we conclude, the message is clear: while navigating the intricacies of health insurance for mental health care can be daunting, equipped with the correct information and resources, one can demystify the process. It’s about empowering individuals to make informed decisions and access the care necessary for mental well-being. The journey may be complicated, but the destination—a state of better mental health—is undoubtedly worth the effort.
-

 Technology8 months ago
Technology8 months ago社工库: Navigating the Depths of Social Engineering Databases
-

 News6 months ago
News6 months agoFinding the Truth Behind a Trails Carolina Death
-

 Education7 months ago
Education7 months agoFortiOS 7.2 – NSE4_FGT-7.2 Free Exam Questions [2023]
-

 Technology3 months ago
Technology3 months agoAmazon’s GPT-55X: A Revolutionary Leap in AI Technology
-

 History & Tradition9 months ago
History & Tradition9 months agoλιβαισ: Unraveling Its Mystique
-

 Education8 months ago
Education8 months agoExploring the Significance of 92career
-

 News8 months ago
News8 months agoClaudia Goldin: A Trailblazer in Understanding Gender Pay Gap
-

 Entertainment7 months ago
Entertainment7 months agoFree Tube Spot: Your Gateway to Endless Entertainment